Staff writer
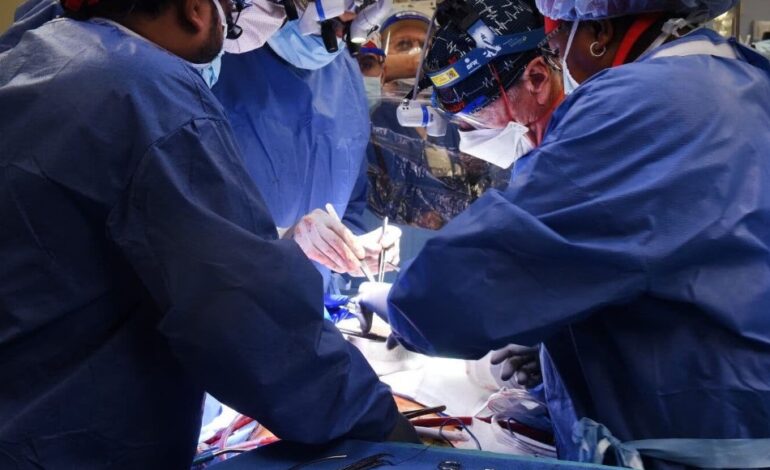
Doctors at the University of Maryland medical center recently transplanted a genetically modified pig’s heart into a human patient.
This was the patient’s last option because he was ineligible for a human heart transplant because of his deteriorated health condition.
It’s now been three days since the high stakes surgery and the patient, now identified as David Bennett is coping well so far.
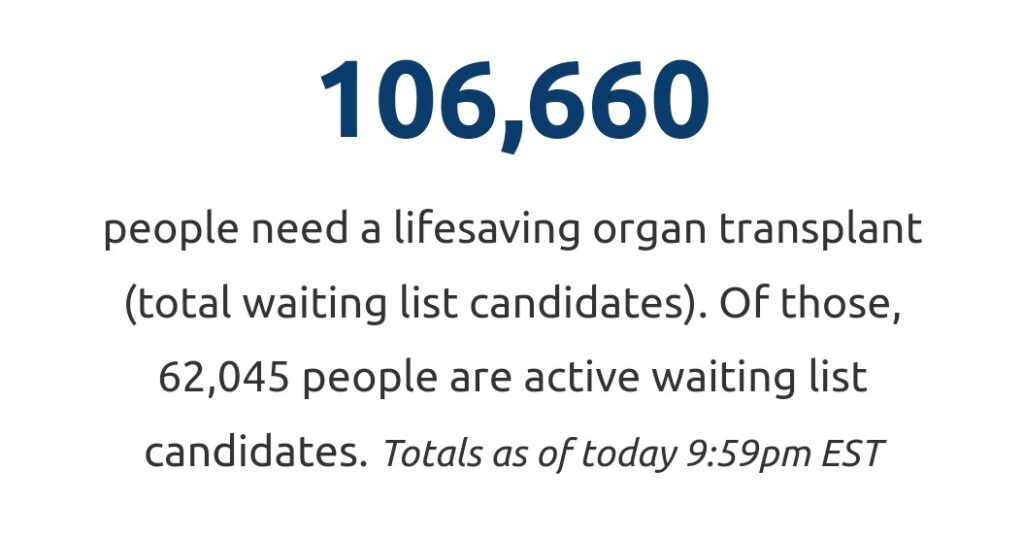
The United Network for Organ Sharing (UNOS) is a non-profit, scientific and educational organization that administers the only Organ Procurement and Transplantation Network in the United States.
On the the organization’s website, there are 62,045 people actively waiting for life saving organs today.
The US had 3,658 in 2020 heart transplants compared to 3,552 in 2019.
The Maryland surgeons said the difference this time was that they had used a heart from a pig that had undergone gene-editing to remove a sugar in its cells that’s responsible for that hyper-fast organ rejection.
“I think you can characterize it as a watershed event,” Dr. David Klassen, UNOS’ chief medical officer, said of the Maryland transplant.
Dr. David Klassen
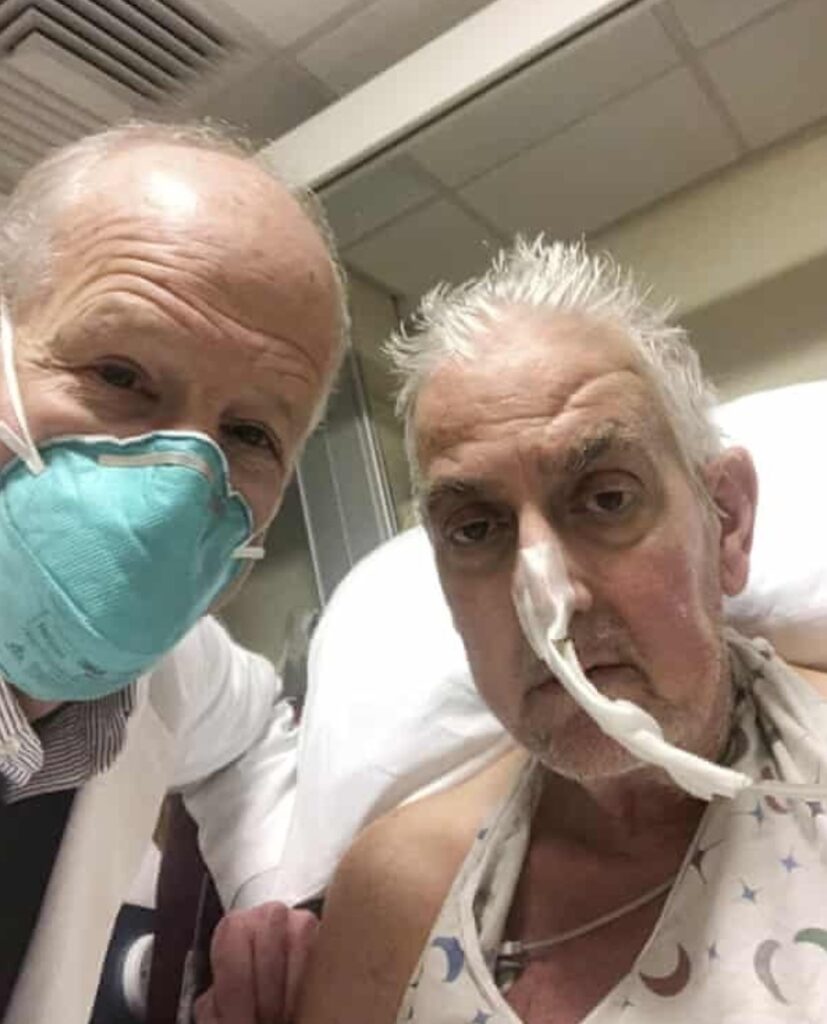
Image credit: AP /courtesy/
There are biotech companies in the US developing pig organs for human transplant. Revivicor, a subsidiary of United Therapeutics provided the gene-edited pig’s heart that was used.
The Food and Drug Administration (FDA), under whose jurisdiction xenotransplantation experiments are performed, gave the green light for the surgery under a “compassionate use” emergency authorization, which available is only available when a patient with a life-threatening condition has no options left.
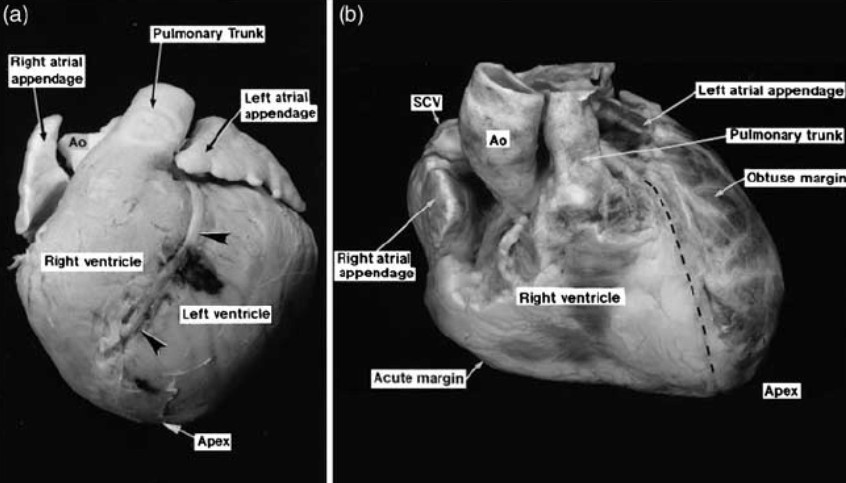
ResearchGate /courtesy/
David Bennett, 57, a handyman, had been advised that there was no guarantee the experiment would work. He was going to die because but he was ineligible for a human heart transplant and had no other options, according to his son.
“It was either die or do this transplant. I want to live. I know it’s a shot in the dark, but it’s my last choice,” Mr. Bennett said just before he went into surgery.
David Bennett
On Monday, Mr. Bennett was breathing on his own while still connected to a heart-lung machine to help his new heart. The medical team will keep him in close observations the next few weeks which are very critical as he makes recovery.
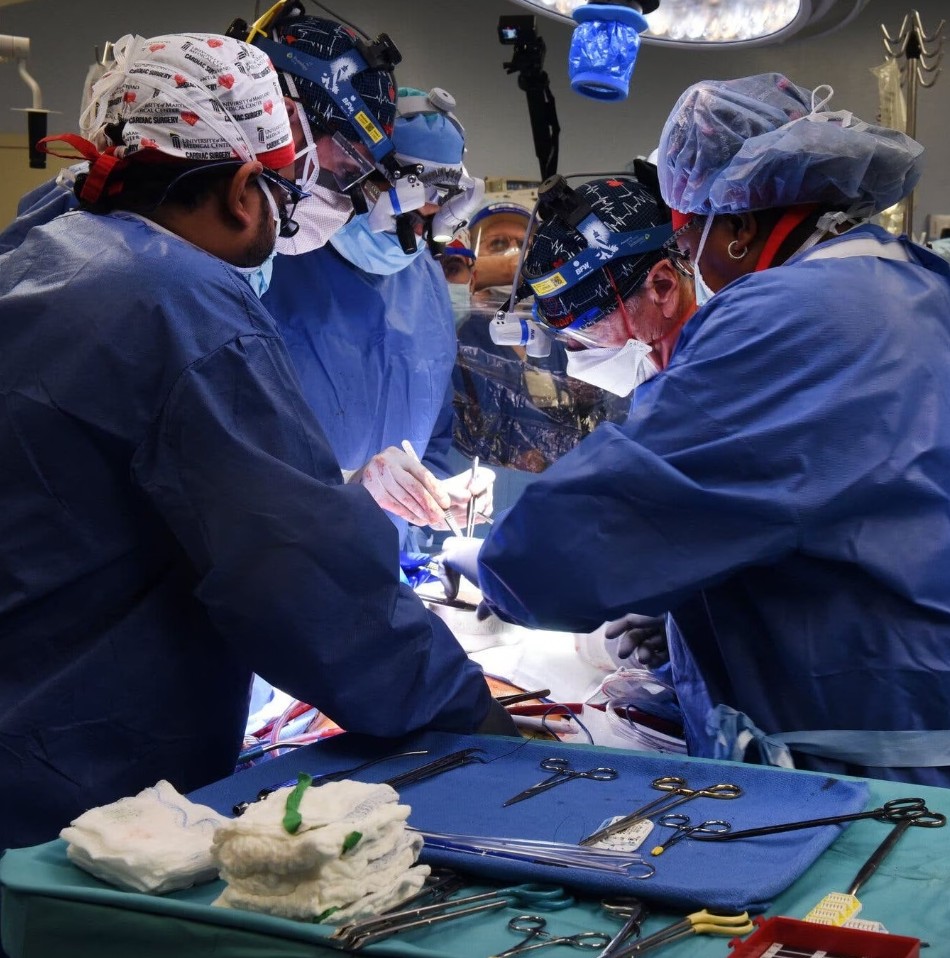
Image: /University of Maryland School of Medicine/
FOOTNOTE:
Xenotransplantation – transplantation of living cells, tissues or organs from one species to another. Such cells, tissues or organs are called xenografts or xenotransplants. (Wikipedia)
RELATED :





Recent Comments