By Faith Nyasuguta
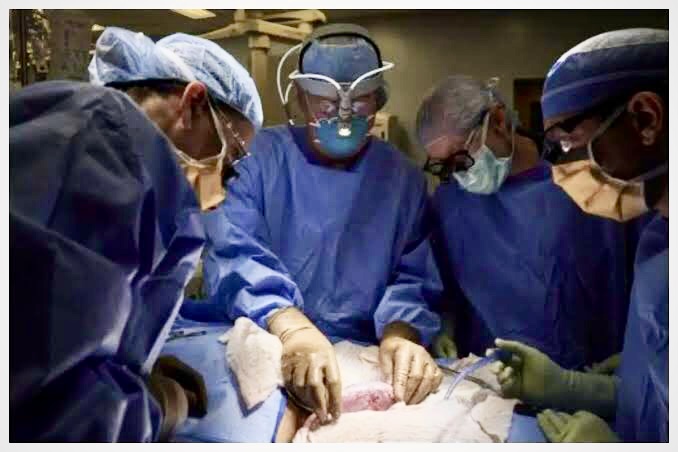
In a ground-breaking procedure, surgeons at a New York City hospital have successfully attached a pig’s kidney to a human being, whose immune system did not immediately reject the organ.
The ingenious operation could be a green light that animals can be used in life-saving transplants.
The beneficiary of the procedure at the NYU Langone Health was a brain-dead woman who received the kidney of a pig with altered genes-in a bid to eliminate a molecule in its tissues renowned for sparking almost immediate rejection- according to Reuters.
Scientists revealed that the family of the patient that had shown signs of kidney dysfunction consented to the procedure before removal from life support.
They kept the woman’s body going on a ventilator after her family agreed to the experiment. She had wished to donate her organs, but they were not suitable for traditional donation.
For three days, researchers could access the kidney since the organ was maintained outside the patient’s body while still attached to her blood vessels.
The study lead, Dr. Robert Montgomery, indicated that the test results from the kidney’s function “looked pretty normal,” adding that the organ produced “the amount of urine that you would expect” from a transplanted human kidney.
Immediately after the transplant, the patient’s abnormal creatinine level — which indicates poor kidney function — returned to normal , he said.
There was also no sign of the strong, immediate rejection seen when unaltered pig kidneys are transplanted into non-human primates.

US ORGAN TRANSPLANTS
Presently, about 107,000 people are awaiting organ transplants in the US with over 90,000 seeking kidney transplants.
However, a person averagely waits for three to five years to get a kidney transplant, the United Network for Organ Sharing says.
Researchers have for decades, been working on using animal organs for human transplants while shielding immediate rejection.
The genetically altered pigs — dubbed GalSafe — were developed by United Therapeutics’ Revivicor subsidiary.
The animals lack a gene that produces alpha-gal, the sugar that sparks an immediate attack from the human immune system.
SIGNIFICANT STEP
In December 2020, the US Food and Drug Administration (FDA) gave a nod to the gene alteration in the pigs as safe for both human food consumption and medicine.
However, the FDA directed that medical products developed from the GalSafe pigs get specific approval from the agency ahead of usage in humans.
“This is an important step forward in realizing the promise of xenotransplantation, which will save thousands of lives each year in the not-too-distant future,” United Therapeutics CEO Martine Rothblatt said in a statement.
“The experiment at NYU should lead the way for trials in patients with end-stage kidney disease, possibly in the next year or two,” Montgomery, a heart transplant recipient said.
However recipients would probably be people with low odds of receiving a human kidney and a poor prognosis on dialysis.

“For a lot of those people, the mortality rate is as high as it is for some cancers, and we don’t think twice about using new drugs and doing new trials (in cancer patients) when it might give them a couple of months more of life,” Montgomery told Reuters.
Dr. Andrew Adams of the University of Minnesota Medical School, said the research is “a significant step” that will reassure patients, researchers and regulators “that we’re moving in the right direction.”
The dream of animal-to-human transplants can be traced back to the 17th century, when animal blood was used for transfusions.
By the 20th century, researchers were attempting transplants of organs from baboons into humans — notably Baby Fae, a dying infant who lived 21 days with a baboon heart.
Scientists then turned from primates to pigs, tinkering with their genes to bridge the species gap. The animals have advantages over primates because they are used for food, so tapping them for organs raises fewer ethical concerns.
Pigs also have large litters, short gestation periods and organs comparable to humans’.




